Weight and EDS and MCAD
This post is apt to be fraught with emotional triggers and landmines due to the nature of the subject itself. Weight loss and management have been a sore point for millions of people for many years, especially in the post war era in the so-called “first world” when big oil and the chemical industry radically changed the face of our modern western food production. And the cosmetic and media industry have established unrealistic standards for women at least at the same time.
I feel strongly that the farther we’ve swung the pendulum to the instant and convenient side in the US at least, the worse our health has become, and the greater our struggle with weight gain in general, everywhere.
All while we continue to simultaneously present increasingly unrealistic beauty standards on magazine covers and in advertisements. So is it any wonder millions are obsessed with their self-image and weight loss, trying to match the standard model?
But many lower and middle class families are trapped in a vicious cycle of working too much to have time to properly prepare a wholesome, nutritious meal from scratch – at least in the west. We have adopted and almost require a dual-income lifestyle to support our consumption habits (both durable goods like computers and gadgets as well as food) and now sky-high housing costs. This leaves many of our able-bodied homemakers of any gender too exhausted and busy to have the time needed to properly prepare a good meal. Not always, but many. (You foodies can sit on your hands here.)
And disabled hypermobile, EDS and MCAD patients with or without fibromyalgia stand even less of a chance, as we are often weaker, fatigue more easily, and often can’t properly process whole or raw foods fully or even at all. Yet we can’t always afford pre-cut or prepared versions either. I’ve been bested by many a chicken and butternut squash myself. And don’t get me started on packaging!
Toss in a myriad of complications we find in the Ehlers-Danlos, hypermobility and MCAD communities, and many struggle to keep any extra weight off, much less eat healthy or well – or even enough sometimes. (Hold that thought.)
What’s a hypermobile body to do?
First off, let me dispel the first big myth: there is no single easy answer to weight management (loss or gain) for ANY one, much less a hypermobile patient. There are no panaceas for any of us, period, we all have very individual metabolisms and methylation cycles as well as detox pathways affecting how we process foods and drugs.
Secondly, there are multiple drivers of weight gain in general that we struggle even more to overcome thanks to lax joints, weak muscles and tendons and chronic fatigue from multiple drivers also. So you’re not going to go away with a single easy answer for your weight loss, sorry. It’s just not that simple. (Sensing a theme I trust.)
Further, some poor folks actually struggle to GAIN weight – something that is all too often overlooked in our image-conscious western media. And many of them have a Hypermobility Spectrum Disorder or form of EDS with comorbid gastroparesis (literally: stomach paralysis and slowed or halted motility) lending to this among other things. I myself was technically “anorexic” (lacking appetite, unable to eat, though not for lack of desire, i.e. “nervosa” in my case) from MCAS three years ago before I figured out I was reacting to chlorine and fluoride in my water. My system was so inflamed I lost most of my appetite. (And I’m a former foodie, so this was unexpected.) I dropped to 106 lbs at 5′ 4″ before I figured it out. (I’m back up to a healthy weight again, no worries.)
Others can and may also have anorexia nervosa (the eating disorder), as well as any other forms of eating disorders too, just to throw another spanner in the works. And yes, in addition to and on top of everything I’ve already mentioned. (We can be a very complex bunch indeed.)
I’ll address some of these causes of weight gain below, but will add that there’s another as yet poorly known cause of unavoidable and intractable weight gain in our community that seems to go hand in hand with this family of connective tissue diseases (hypermobility, EDS and MCAD) that is rarely recognized still called:
While it seems to strike most predominantly in women, men can and do have it also. It is an actual adipose (fat) tissue disorder that causes truly unavoidable weight gain no matter how healthy (nutrient dense) and few calories you eat and apparently no matter how much you exercise. You may lose “regular” fat aka “obesity” from dieting and exercise, but this won’t comprise the majority of your fat with this condition. It’s probably part of what was “eating” Gilbert Grape’s mother (although she is portrayed as just having an eating problem), and is afflicting one of my best friends who eats less than I do, no kidding. Yet somehow she weighs three times more no matter how carefully she eats.
I’m deeply convinced that what is now called “Dercum’s Disease” is really just a case of lipedema with as yet unrecognized or identified clinical MCAS on the side. But that’s just my unprofessional opine of course. Articles like this one and this one are what are leading me to increasingly think this along with my own experience with stress-induced inflammation and observation of many online.
Unfortunately for this latter group, there isn’t a lot yet to be done besides continuing to try to eat as nutrient dense and healthfully as possible according to your body’s sensitivities. Many find they are gluten sensitive also, if not outright celiac which seems to also lend to weight-gain, possibly from secondary Hashimoto’s disease or other hypothyroidism.
So as you can see there are several reasons for seemingly intractable (unavoidable, hard to shake) weight gain in women and some men and others that have nothing to do with your caloric intake aside from quality and gluten content, and a healthy lifestyle. Sure, it’s worth trying to diet and exercise and staying as healthy as you can, but some people will just plain gain weight despite all their best efforts to not do so. Toss in joint laxity and hypermobility if not also MCAS, and it’s very hard to “exercise” to any significant degree for some further compounding the issue. This should be raising a red flag for your doctors to look further, but few do.
This, and many other reasons including just plain personal agency of one’s body are a couple of really good reasons for everyone to stop fat and body-shaming yesterday. Is there a subset who could use some dietary help and portion control? Sure. But I’m increasingly convinced “true obesity”, meaning excess weight above mean BMI from over-eating and lack of exercise is actually a minority of the cases in overweight or fat people we see now. And let’s face it, anyone who overeats probably has other issues that can use support as well such as depression and other eating disorders from a variety of other causes they would rather not have.
And yes, we now prefer the term fat to obese, or bariatric, which is simply medical speak for the same thing, which pathologizes our bodies, adding a layer of judgment. I know my friend didn’t ask to be the weight she is, but not one doctor recognized any of her underlying conditions all these years, just writing her off as “obese”, and assuming she ate too much. If they only knew!
But this is why I’m writing this post – to help raise awareness of the multiple drivers of weight gain in the hypermobile population, whether you have an officially recognized form of the “Ehlers-Danlos syndromes” or not. It appears that whatever is driving the Hypermobility Spectrum Disorders (think “subclinical EDS” now since 2017) lends to this for as yet unknown reasons. I know at least one doctor in Arizona who is aware of and working on trying to suss this out as I type. We just need to clone them. And raise awareness among everyone else.
And again, some poor folks literally struggle to gain weight, and gain strength. I think this can be from multiple drivers again stemming from both a connective tissue disorder (HSD or EDS etc.), and possibly biochemical or hormonal imbalances or trouble. (Addison’s, gastroparesis.) Some people vomit every time they impinge their vagus nerve. Others react to almost everything they eat, and sometimes even just to the act of eating itself due to their MCAS or mastocytosis. They may end up on total parenteral nutrition, or G- or J-tubes to maintain their health at all. There is no true cure for gastroparesis itself, but Crystal Saltrelli has uncovered many helpful solutions.
Should you just eat freely then if you’re heavy, since it doesn’t matter? I won’t stop you. But I would still urge doing your best to eat as nutrient dense and low-inflammatory for YOU as possible, in all cases. Avoiding known MCAS triggers will help lower your histamine levels and keep that over all inflammation down. And definitely avoid gluten if you are or suspect you may be celiac. (You may be surprised.)
I personally do best on a mostly paleo semi-ketogenic diet I’ve adapted from the GAPS diet I first tried successfully in 2013. I’m so grateful to have found something that works more than not for me, although I remain in constant GI pain and mildly inflamed at all times still. I am managing and can work again, including around my diet. But we all have to “thread our own needles” so to speak, and find what works for each of us based on our body metabolisms and chemistry as mentioned above.
No, the holidays don’t help! Just start where you’re at, with what you can. Even one small change a week or even per month will be a step in the right direction, right? And yes, it’s much harder for families to make these changes than individuals like myself. No one is pressing me to eat things I shouldn’t thankfully at least at home. They still do when “out”, which is very frustrating. But I’m slowly prevailing, and we all will, one meal at a time. At least you know you’re not alone!
To your health,
Jan



Hi- you make some very good points and I agree with you on the connection you are making between hyper mobile, EDS, Lipedema, and Dercum’s Disease and MCAS, as I suspect the same. I am 63 years old and always knew something was wrong. I always exercised and ate healthy and yet my body never reflected those efforts. I was recently (2017) diagnosed with Lipedema Stage 2/3 and Dercum’s Disease and Lymphedema and hyper mobile. Just this past week I was diagnosed with EDS & MCAS. The dots are being connected, and it is becoming more clear of the relationship of these disease states.
I’m so sorry you’ve had to experience these conditions all together, but… I’m glad my post resonated with you. I do see it increasingly in the groups, now that it’s on my radar. It’s hardest to watch those whom I consider to be in the earliest stages continue to deny the possibility because… like all of our conditions, they only see or believe in the grossest signs of the rarest/worst forms or stages. You don’t start at stage IV!
I’m also increasingly curiuos if mast cells don’t play a role in this clearly inflammatory disease path, along with some particular mutation that lends to it. That’s my gut hunch anyway. I’d love to hear if Dr. Afrin (MCAD specialist in US) has seen or noticed a relatively high incidence in his clinic…
Thanks for including those of us who struggle to weigh enough in your post. I believe it carries just as many health issues and inconveniences as being overweight, but many laugh at that idea, since being skinny is the false epitome of perfection these days.
I hadn’t heard of Lipedema or Dercum’s Disease. Thank you. Though I obviously don’t have that, I always like to be as aware as I can for my own knowledge and to help guide others toward information.
You’re quite welcome. As a longtime support group leader I’ve met patients suffering from both extremes of the weight spectrum and some of my best friends are suffering from both extremes – inability to gain as much as inability to lose weight.
TW: discussion of death
And the leading causes of death I’ve seen so far have been from severe gastroparesis driven malnutrition, followed by complications of spinal fusion and Chiari decompression surgeries at the hands of inexperienced surgeons. So it’s real to me. Glad you felt recognized in my post and it resonated. It’s not a trivial matter. I wish you luck finding your solution.
And I just stumbled across this via Twitter today… low Vit D levels in moms can lead to obesity in some children… hmmm… now my brain is running further afield and wondering if this doens’t also play a role in the development of lipedema in some?
“Animal studies have shown that vitamin D suppresses pre-fat cells (adipocytes) from maturing into fat cells. Test tube studies of human fat cells also showed that vitamin D may hinder pre-fat cells from turning into fat cells.”
https://www.sciencedaily.com/releases/2018/02/180213145823.htm
Really interesting post, Jan! I was always extremely slim until 10 years ago when all my EDS symptoms and back problems increased and I was prescribed Pregabalin & mirtazepine for chronic nerve pain. Now my hospice patients had always said that pregabalin caused weight gain, but until you actually experience yourself you can’t understand. Obviously reduced mobility doesn’t help either but I ensured I reduced my calorie intake knowing weight gain to be a side effect, but I think I only had to look at the drugs- and I didn’t gain as much as some people (about 3.5 stone total I think). It is interesting to consider the science behind this and I think you are right to consider MCAS in the equation. Ironically due to increased gut problems/gastroparesis and dysautonomia I have now lost most of the weight and whilst I am delighted to be back in my old clothes, it isn’t a healthy way to do it!! Will def share this post, C x
Thank you for adding this additional driver of weight gain in some Claire: many of our medications (including antihistamines) can also lend to seemingly unavoidable weight gain. I’m sorry your weight loss also came from the very devastating highly comorbid gastroparesis: having seen many lose their lives to it, I can’t agree more that it is definitely NOT a good reason to be losing weight. 🙁 Best of luck to you.
How did you lose the weight? What drug helped?
Thanks to a follower on Twitter, I want to also add PCOS and it’s equally deceptive cohort Lipodystrophy as additional comorbid causes of unavoidable weight gain or loss. They both involve insulin resistance too. Check them out.
Hi there.
Long time weight gainer.. going potty as only consume around 1500 cals a day at a push.
EDS, PCOS, RA, Depression, Vitiligo, IBS, Tinitis – just had a biopsy to test properly for celiac as my anemia and fatigue is raging out of control.
I’m fairly sure I have some sort of MCAS too that has been shoved to one side and called IBS with unexplained itching.
Currently going back to as gluten free as poss (just realised my oats were not gluten free damnit!) Even if my tests come back negative to celiac as it’s the ONLY thing that has helped combat the anemia at all.
I really struggle mentally with the weight thing though, although it is the least of my worries I guess.
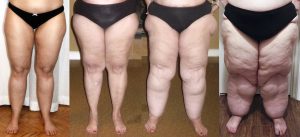
My lower body resembles stage 1 I guess in those pics heading towards the second pic rapidly.
I did try keto diet for a short while and put on a few pounds.
I’m well over 200 lbs I think but the inflammatory pain and fatigue is too much to exercise. Anyone have any ideas? Also am fed up of celiac people only being thought of as underweight.
Hi Clair, I’m so glad my post resonated with you. And… trust your gut! You are more than likely right on all counts, truly. I agree about likely having unrecognized MCAS (the high histamine from it makes us itch). I’ve yet to meet a hypermobile patient of any flavor who doesn’t after drilling down far enough.
I also agree about the possible celiac – I’m finding that fairly comorbid also. In fact, the only reason I think I’m not officially celiac is because I think I have selective IgA deficiency. And you can only be Celiac with sufficient IgA. So I’ll never test positive. But I’m definitely gluten-sensitive (IgG). So I avoid it as much as I can. (Not enough!)
And I thoroughly agree celiac can lend to weight GAIN as well as loss. My best friend shares that experience. As well as one of the worst cases of lipedema to ever start recovering her PT has ever seen. You can learn more here: http://morethanfat.com.
Anyway, I agree, it can seem like weight is not that important, and in some ways it’s not. But do keep an eye on any possibly emerging lipedema. It turns out it can be kept down to a dull roar so you don’t end up like my friend. It sounds like you’re already on the right track for that.
I’m just now starting to use this video for myself to start working out in my home more now – a little more slowly and gently to start. (Adapt to your needs too.) https://youtu.be/X3q5e1pV4pc
Hope that helps. Remember, you’re not losing your mind – just your body! And we can get that back too in time. (I couldn’t even walk 7 years ago and can again now at 52.) Hang in there!
Someone just sent me this great video series featuring Lipedema Doc Dr. Karen Herbst of Arizona and a generous brave patient modeling how to suspect and diagnose Lipedema here:
https://youtu.be/x47UhXT3l2M
I’m really glad to see they included her obvious (to me) comorbid hypermobility syndrome as well.
I’ve been struggling so long to try to lose weight, it’s a life long project. I suspect lipedema. I have terrible cellulite on my lower half and have since I was around 8, when my struggle with weight began. My mother was the same. I’m a trifecta zebra with EDS, POTS and MCAS and I’m pretty sure she was, too. I’ve wondered for a while if lipedema might be the problem. I’ve lost 50 lbs over the last two years, maybe in part because I’ve developed gastroparesis, but it stopped about 6 months ago and nothing more has happened. I wonder if perhaps I was losing because I was blasting. I quit blasting regularly because I no longer needed it to control pain, but maybe I should go back and see if it helps. It’s definitely helped with the lipedema/cellulite. I worry about eventually becoming malnourished with gp, but I worry more about what 260 lbs does to my joints and I don’t know that a lack of weight loss is going to keep me from malnourishment or just keep doctors from taking it seriously. I’m already so deficient in vitamin A, my vision is at risk.
So sorry for your weight loss struggles, but I’m really glad you feel you may have some answers about your various symptoms and issues. I don’t know what blasting is – I’m guessing it has somethign to do with reducing cellulite, but it does sound like it may have been helping you.
I also find managing the highly comorbid secondary lymphedema we often also get with any extra weight (from lipedema or not) is crucial. I think our lymph systems are floppy too, just like the rest of us from faulty collagen. So it stands to reason we may have a lot of trouble with this.
Gastroparesis is another whole bag of trouble all by itself. Like everything that plagues us, I think it has both bio-mechanical and bio-chemical drivers, such that there is also no single easy answer or “cure” for it. I think I”m lucky to only have mostly bio-chemical drivers (essentially, GI inflammation) so far, touch wood. But I’ve known too many to suffer from literal malnutrition despite caloric intake due to true neuropathic slowed motility. I hope you can prevail. And keep your nutrition up in all cases! Good luck. x
Do you know of any woman with EDS spectrum disorder who has been morbidly obese then lost weight by any means? Did all the skin retract? Did the skin and fibrosis on the bottom of the body fail to retract giving a disproportion? Thank you for the nice article!
As a matter of fact I do know of some. My best friend who has stage IV Lipo-lymphedema, Esther, is just now uncovering one of the only ways to lose weight she has ever found to work: a ketogenic diet. I met her over 20 years ago at work, and she was morbidly obese then despite eating less than I did. (I’ve never gone over 140 lbs.) But her weight slowly and steadily ballooned to over 500 lbs this last year when she finally stumbled onto keto (plus going gluten free as a celiac) and it’s been working wonders for her. She’s lost over 60 pounds in the last year, and without being able to exercise at all yet. (Long story, she should tell you herself.) You can see her background story for yourself here:
https://morethanfat.com/my-story-with-lipedema
That said, she’s been telling me that she also just learned in the keto dieting group she’s in on Facebook that people are having the greatest success with skin reduction along with the weight loss through intermittent fasting. It’s thought that this induces autophagy, which helps the body to literally remove old unwanted cells, and thus you have a lot less excess in the process. (The skin sort of disappears in sync with the fat loss this way.) It’s a strict process, or at least the schedule needs to be strict. And I would recommend only doing it under a doctor’s supervision or with your doctor’s blessing of course.
It’s an honor to have you comment on my blog, Dr. Herbst! Your reputation as the only (or best) lipedema specialist in the US definitely precedes you! And I uncover more lipedema patients in the HSD/EDS community every time I share this post, so you’re in very high demand as you know. Thanks for all you do for the community!
Jan Groh, author
Wow! Loved how you shared the weight struggles many of us have along with our EDS!
I had the gastric sleeve surgery about 2 years ago… before I was diagnosed with EDS (diagnosed almost at 40 years old)… was initially “successful” – losing 80 lbs. However, I was ingesting 800 calories or less per day. I was living on protein shakes and was absolutely miserable. As soon as I started adding solid food back into my mainly vegetarian (sometimes pescatarian) low-carb diet, the weight came back. Now, I’ve regained nearly all of the weight lost – while maintaining a 1000-1200 calorie diet. I don’t eat fried foods, red meat, pork, frozen entrees, etc. It makes zero sense as to why others who eat much more than I do, weigh significantly less. It’s infuriating.
Thankfully – based on information posted to your site and to the Facebook group, I am armed with more information. I also have new health care providers/specialists at the University of Iowa – and we are exploring whether I also have MCAS and lipedema. (I already have a whole host of other diagnoses – am grateful to the U of I for helping me finally get some answers!)
Thank you @Jandroid for your service to our community! For me – the resources your site references, the Facebook group, and the topics you explore – have increased my knowledge and I would dare say, has improved my life!
Aw, you’re very welcome Kim! I’m so glad I could help arm you with a few more insights and possible leads to help regulate or understand your weight gain going forward. Sorry for your painful journey – including the surgery. And, love yourself and your body as you are, right? (Speaking to myself too here, mind.) Glad you’re finding the support you need in my group and here. Good luck on the rest of your journey!
Jandroid 🙂
This is a great blog post, thank you for bringing attention to the weight issues that people with EDS face, both to lose weight and to gain weight. I love that you touched on both issues.
You’re most welcome, glad it resonated with you, thoguh sorry for your issues. I have dear friends who struggle with both sides of the equation badly, literally fighting for their lives, so I was aware of both. And, I feel it helps to show how widely varying EDS and Hypermobility Spectrum Disorders can present to doctors, so they keep an open mind about what to look for. There is absolutely no “standard” EDS patient, period, IMHO.
Jan
Good read and really goes with what I have been thoroughly digging through to explain the unexplainable. To make things semi short I have MCAS, hypermobile, have many EDS symptoms yet many Marfan (I think mom carries EDS and Marfan (have a cousin diagnosed Marfan)…dad is very much Marfan symptom but no definitive testing)
But I digress I had nothing but GI problems since birth….along with weight. At 5 I was 75lbs and 4ft tall. I was 5’10 and 220 by 10. Thing is mom is 5’2 and dad is 6’4 so with the drastic height differences obviously noticing somethings is ignored. My siblings are 5ft and 5’7. But they do not have a weight issue like I did. By the time I was 21 I was 400lbs. Didnt matter I didnt eat much, was insanely active etc etc. There was no reason but to Drs I just ate to much. I never was diagnosed with lipodemia, as I never had the lumps. Well at 22 I finally had enough I had weightloss surgery but not the typical. I had the most techinically challenging one. Gastric reduction with duodeanal switch. Well 14 years later its kept the weight at bay. As long as I am smart with my eating. The thing about the DS that sold me is at the time I already had issues with many pain meds and artificial sweeteners/and non traditional sweeteners. And the DS allowed me to eat normal/more varied and take the few pain meds I could. But I also had my DS long before other things rose up. Yes losing the weight helped me drastically. But at one point I got to my lowest weight (very very manual labor based job) and my symptoms got bad real bad, anaphylectic shock multiple times bad. Got new job gained some weight back (and then some from having to me on nights for a year). But Ive found a happy place with my weight and with my med regamines to be pretty stable now. But honestly I credit my surgery for being able to control things better. I was never an over eater or a bad eater. Now its just to get a definite diagnosis to help my siblings and myself better.
Wow, thank you for sharing that amazing weight control odyssey with us! And glad to know that DS surgery worked for you. Every body is different. You may still have lipedema – the lumps go more with Dercum’s disease, I think. But, the key is that you’ve found a way to stay balanced that works for YOU and that is fantastic.
Also, the height difference you’re describing is common in EDS families. We all seem to have some really tall and/or some really short folks all mixed together. And many will also have really long wing span to height ratios. That is, your wing span (arm span) is longer than you are tall. They call this “marfanoid habitus” which would match the Marfan history in your family also. Glad my article resonated! Cheers.
Thank you so much for this post! I have a very peculiar (or maybe not so peculiar after reading the post and comments here) history with weight. I started life as a beanpole, much taller than my peers & very thin. Suddenly at age 8, I stopped growing taller, but my weight continued to increase. I seemed to start a very early puberty, & then went on to gain quite a significant amount of weight, which was then what was used to explain the early puberty (though it actually came after). I long suffered from joint pain, even as a child, I was ridiculously flexible & constantly injuring myself, and I constantly had digestive problems. I began to grow a bit taller at age 10, but I stopped completely by 13. My digestive issues & pain continued to plague me. It got to the point where literally everything made my sick, & I could no longer eat without vomiting. I was diagnosed with celiac disease at age 15. Going gluten free helped significantly, & I seemed to lose a lot of weight after doing so, as I was mainly just extremely bloated & inflamed from the gluten. Eventually though, it became difficult to keep any weight on, and into my 20’s I struggled terribly with chronic pain, migraines, headaches, and I could barely eat. I already knew I likely had hyper-mobile type EDS from reading about the diagnostic criteria myself (& from my mom & siblings clearly having it as well), but doctors wouldn’t take me seriously until just a couple of years ago. Medical professionals now believe I have POTS & MCAD as well, & I swear the mast cell issues can drastically change my symptoms based on what I eat. With physical therapy & chiropractic care I’ve improved drastically, but oddly enough, I’ve had a sudden switch in weight this year with just one isolated exposure to gluten. I haven’t eaten wheat since I was 15, & I’m 28 now. I had the odd glutening incidents over the years with very small amounts, but nothing too serious. However, earlier this year I accidentally had a terrible mix up, & ate a full food item containing gluten. After this I could literally not eat any food for nearly two weeks without extreme stomach bloating (I thought my stomach might literally explode by the looks & feeling of it, I looked 9 months pregnant), so I was forced to go on a liquid diet & slowly reintegrate solid foods. I tried to low FOD-MAP diet with some good results, & I was able to reintegrate many foods. However, after this glutening incident, it’s like my entire body & metabolism have changed, & I started packing on the pounds. After years of struggling to gain a pound, I gained 20 pounds over the course of a month for no apparent reason. I did not significantly change my exercise habits, & I didn’t eat any more or worse than before, yet somehow I looked completely puffy & bloated with weight gain. I thought after waiting months it would likely stabilize, but so far I haven’t had such luck. With working out more than I already do being very difficult for me, I can’t seem to workout enough to put even a tiny dent into this new weight, so I’ve basically had to just except it as my new normal. I’m really not happy with my bloated body now, but I feel powerless to change it. It’s so frustrating to experience a body that goes from digesting little to nothing & being too thin to suddenly becoming a bloated, puffy heavier person. I just want a balanced body, but none of it feels in my control. When it comes to my weigh, it feels like I’m at my own bodies whim.
Wow, thank you for sharing that very painful journey with Celiac disease and your variable weight. I’m going to make sure my dear friend and author of http://morethanfat.com reads this as you’ve described the latter half of her life quite well – experiencing truly unavoidable weight gain, but long before she knew she was celiac. If you do have lipedema, you’ll want to wrangle it sooner than later, and it involves more than diet.
I’m so sorry you feel yourself ballooning despite eating so carefully! I’ve just gained the most weight I’ve ever had in about a six to nine month period, but I’ve topped out after 30 lbs and seem to be holding here at least at 52. (And I feel like I could lose a couple if I could exercise more than I am now, and may. I’m blaming menopause and may a sluggish thyroid despite my tests contradicting this.) My friend could not lose a pound for love nor money until she went completely gluten free also, and ultimately keto in her 50s. She has since lost over 100 lbs, thankfully, as she was headed to immobility.
I pray you get some answers – and I can’t help wondering how many with lipedema may also be Celiac and vice versa. Though I do know some thin Celiacs too – it seems to go to either extreme, vs the middle ground. (I’m not Celiac but I’m IgG sensitive.) You might check back in your family history, to see if you find any signs of either lipedema or Dercum’s and/or Celiac on either side. It can be in any gender, though seems to express more often in women. Best of luck and hope to you.
I am an occupational therapist working with 2 brothers with EDS. They are 7,9 years. Both have gained a lot of weight over the past year. Both are picky eaters. I am trying to figure out if there is a way to help them. activity is limited by fatigue. I just saw something about the Keto diet. Wonder if that would help them.
Of course, I can’t say for sure, as I’m both a) not a doctor or nutritionist, nor b) their doctor, and c) even if I was, I can’t give advice over the internet. But… my personal unprofessional hunch and opinion is yes, I think keto might be worth trying (with their doctor’s approval and parents’ too of course). It’s not for everyone, but… I’ve seen a fair percentage of the EDS and neurodivergent community benefit from a keto diet. Both in terms of weight loss, and… improved cognition and health. (A high fat diet can help with epilepsy too. Key is being low carb at the same time.)
That said, if they are picky eaters, it’s hard to say how manageable this plan could be for them. But, maybe you could plant the seed of the idea now, and wait patiently for it to bloom?
I only skimmed the article (I’m in eating disorder recovery), but I did see a comment that someone assuming you had to be fat to have lipedema. My mom could get down to 90 pounds with lipedema because her lipedema was only in her thighs. She would be skin and bones elsewhere, but thighs still round. If you image search for anorexia and lipedema there’s an example picture.
Also I wanted to note that lipedema is not ob*sity, it’s a different style of fat cell altogether. (I know the article is older and lipedema research is progressing quickly).
Thank you for highlighting this condition! I knew I was dx with lipedema in 2015, but just got the hEDS diagnosis this month, and with probably 10% AFAB people thought to have lipedema it is just SO underdiagnosed. The US consensus paper noted a full half of lipedema patients have hypermobile joints.
Thank you for your feedback and additional insight into lipedema also being possible in much thinner bodies. I did clarify that lipedema fat is NOT the same as obesity in my article (maybe you missed that in your skim) but… it doesn’t hurt to emphasize it. Yes, most with lipedema are fat, but… I’m increasingly convinced that it’s yet another form of connective tissue disorder that is highly comorbid with the hypermobile community for whatever reason. Is it mast cell driven? Or a specific additional genetic defect we haven’t seen? Anyway congrats on getting your hEDS recognized finally too. And again thanks for this additional insight.
ETA a link to my friend’s great page that shares the same insight here: https://morethanfat.com/what-is-lipedema
Thank you for this article. Even though I don’t know how to feel better, it’s helpful to hear about other people with similar problems. I watched the YouTube interview with Dr. Herbst and I was happily surprised (delighted? feels like not quite the right word) to hear her ask about comorbidities. I too had a tonsillectomy after recurrent neck infections/swollen lymph nodes in the neck. Got shuttled to gifted-and-talented rather than anyone noticing/helping with neurodiversity. Exercise-induced anaphylaxis (which I now think was just early MCAS) in my 20s. Hypermobility syndrome and MCAS diagnosis in my 30s. Over a decade on Weight Watchers and haven’t made a dent in my legs–just gave myself anemia and hypothyroid problems from starving myself for a decade. Great. Maybe now that I can see it’s all related to my lymph system, I can actually improve. But I won’t hold my breath.
Sorry for my delayed response. Thanks for commenting. I’m so sorry for your challenging journey but so glad you are also finding the right answers, slowly but surely. I swear I’m going to rename this Gaslighter’s Syndrome before I’m done – we are gaslit and dismissed and fat shamed so much! Also, I just (just) learned form this yera’s EDS Global conference about a new to me fascial release therapy called “Counter Strain”. (No affiliation.) And they raved about the results in hEDS and HSD patients and mentioned it can help with lymph drainage!~! You better believe my ears perked up at that. But, she also said in the Q&A after to go low and slow at first, as it will release a load of toxins from your fascia that you will then need to drain away in your lymphatic system. But, that it can help you do that, ultimately. (So, lightly mixed message.) Anyway, along with manual lymph massage maybe it could help a little? Learn more about it here: https://counterstrain.com